Researchers Investigate How to Make Donated Organs Compatible With Any Blood Type
Researchers Investigate How to Make Donated Organs Compatible With Any Blood Type.
A new study published this month in Science Translational Medicine is suggesting that it may be possible to convert blood types safely in donor organs intended for transplantation.
If this becomes commonplace, organ donation could be far more common and accessible.
Traditionally the compatibility of blood types between donor and recipient has been vital to the success of organ transplants. This has led to long waitlists, inequiable organ allocation, and a high risk of mortality for patients on the waitlist.
How has organ donation worked historically?
One of the key components to organ donation and transplant is blood matching. Each person has a specific blood type from four main ones. The eight most common blood types are A+, A-, B+, B-, O+, O-, AB+, AB-.
These are based on whether or not red blood cells have certain proteins, called antigens. Blood has to be compatible between donor and recipient. Otherwise, the receiving body’s immune system will interpret the new blood type as foreign and will reject the new organ.
But people with Type O blood are called universal donors. These people lack antigens which can trigger an immune response.
Similarly, Type AB blood is known as the universal recipient, meaning they can receive blood and organ donations from all blood types.
These blood types aren’t as common as Type A and B, though, which is one of the reasons why organ donation waitlists grow so long.
“With the current matching system, wait times can be considerably longer for patients who need a transplant depending on their blood type,” said Dr. Marcelo Cypel, Surgical Director of the Ajmera Transplant Center and the senior author of the study, in a statement.
According to Dr. Aizhou Wang, Scientific Associate at Cypel’s lab and first author of the study, patients who have Type O blood and require a lung transplant experience a 20 percent increase in mortality while waiting for a matched organ.
A universal Type O
The study, conducted by the Latner Thoracic Surgery Research Laboratories and UHN’s Ajmera Transplant Center, explores the possibility of creating universal Type O organs, which could improve fairness in determining who gets an organ donation.
Universal type O organs would also decrease mortality for patients on the waitlist. Right now, the average time frame for waiting for a kidney transplant, for example, can be 3 to 5 years, and even longer in certain parts of the country.
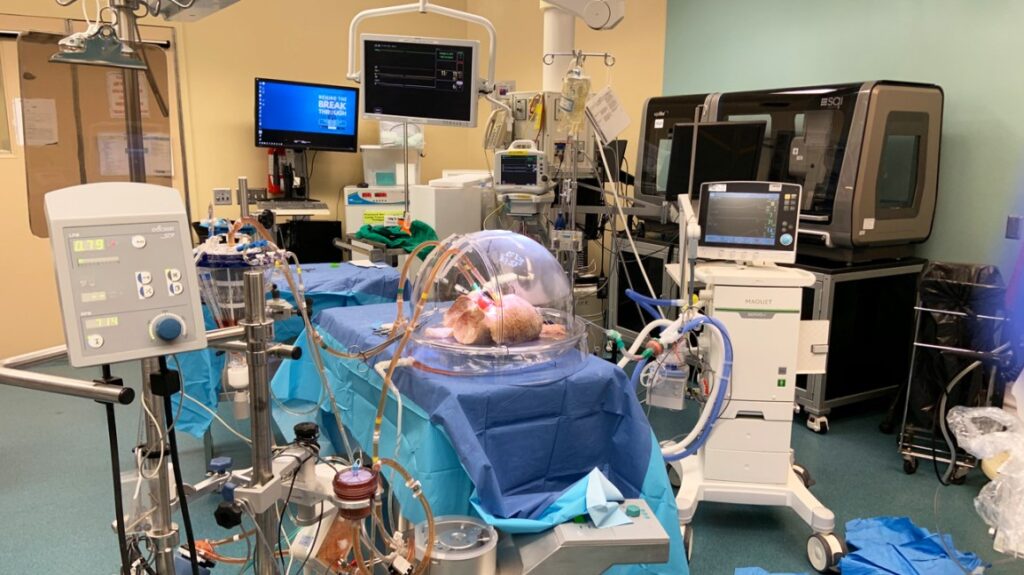
The study used the Ex Vivo Lung Perfusion (EVLP) system as the platform for the treatment. It took human donor lungs that were not suitable for transplantation from Type A donors and put them through the EVLP circuit.
One lung was treated with a group of enzymes to clear the antigens from the organ, while the other lung, from the same donor, remained untreated. Each lung was tested with the addition of Type O blood with high concentrations of anti-A antibodies in order to simulate an ABO incompatible transplant.
What the results showed was that the treated lungs were tolerated, while the untreated ones showed signs of rejections.
If this research proves to be effective in clinical trials, the results could mean that organs from one blood type could be treated so that they can be used in a recipient of a different blood type.
“This has a potential to allow non-blood type compatible transplants to be performed for those having difficulty getting a match,” said Dr. Bryan Whitson, cardiothoracic surgeon at the Ohio State University Wexner Medical Center and professor of surgery at Ohio State University College of Medicine. Whitson was not affiliated with the study.
The next steps
Whitson said more research is needed to verify that this method of treating an organ can work in people.
“We are moving more toward personalized medicine and engineering a donor organ for a specific recipient’s biology,” said Whitson. “The next step is proceeding with transplantation in large animals and then people.”
The team of researchers will next work on a proposal for a clinical trial within the next year to a year and a half.